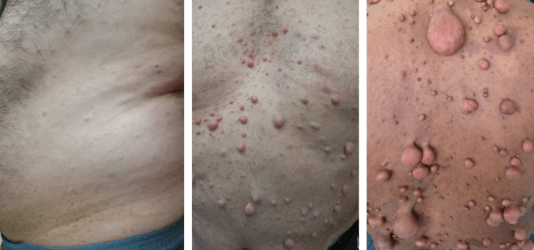
You may have noticed café-au-lait spots, freckling in unusual places, or bumps along nerves and wondered what they mean. Neurofibromatosis type 1 (NF1) is a genetic disorder that causes changes in skin pigmentation and the growth of benign nerve tumors, and it can affect learning, bones, and other parts of the nervous system.
This post What Is NF1 Disease will walk you through what causes NF1 at the genetic level, how the condition typically shows up across different ages, and which symptoms merit medical attention. Expect clear explanations of the biology behind NF1, common signs to watch for, and what diagnostic and care options look like so you can understand the condition and its implications for yourself or someone you care about.
Genetic Causes and Pathophysiology
NF1 results from inherited or new mutations in a single tumor suppressor gene and leads to loss of a protein that controls cell growth. These genetic changes drive the formation of nerve sheath tumors and contribute to pigment, skeletal, and vascular abnormalities.
NF1 Gene Mutations
The NF1 gene, located on chromosome 17, encodes neurofibromin. You usually inherit one mutated copy in an autosomal dominant pattern, giving each child a 50% risk if a parent is affected.
About half of cases arise from spontaneous (de novo) mutations, so a family history may be absent.
Mutations are highly variable: nonsense, frameshift, splice-site, large deletions, and missense changes all occur.
Certain large deletions correlate with more severe manifestations, such as earlier tumor burden and cognitive effects. Genetic testing detects most pathogenic variants but mosaicism can complicate interpretation.
Cellular Effects of Neurofibromin Loss
Neurofibromin acts primarily as a GTPase-activating protein (GAP) for RAS proteins, turning active RAS-GTP into inactive RAS-GDP. When neurofibromin is reduced or absent, RAS signaling stays elevated, driving increased cell proliferation and survival.
This dysregulated RAS–MAPK and PI3K–AKT pathway activity underlies tumor formation (cutaneous neurofibromas, plexiform neurofibromas) and increases risk for malignant peripheral nerve sheath tumors.
Neurofibromin also influences cytoskeletal dynamics and cAMP signaling, which helps explain non-tumor features you may see — learning difficulties, bone dysplasia, and vascular lesions.
Loss of heterozygosity in Schwann cell precursors often precedes neurofibroma development, while the tumor microenvironment (mast cells, fibroblasts) further promotes growth.
See also: Plumber Near Me Emergency Repairs and Same‑Day Service Guide
Key Symptoms and Clinical Presentation
You may notice early skin findings, changes in vision or learning, and growth of benign nerve tumors. These issues often appear in childhood and can evolve throughout life, so monitoring and targeted care matter.
Distinctive Skin Changes
You will commonly see multiple café-au-lait macules—flat, light-brown spots—present at birth or appearing in infancy. Having six or more café-au-lait spots larger than 5 mm in young children or larger than 15 mm in adolescents is a diagnostic clue.
Freckling in unusual places, especially the armpits (axillary) and groin (inguinal), often develops by school age. You may also notice discrete, soft bumps under the skin called cutaneous neurofibromas that increase in number at puberty and during pregnancy.
Pigmentary features vary in size and number between people. Dermatologic findings are often the first signs you or a clinician will use to suspect NF1.
Neurological Manifestations
You may experience learning disabilities, attention deficits, or developmental delays; about half of people with NF1 have some cognitive or behavioral challenges. Motor milestones can be normal, but specific deficits in visuospatial skills and executive function are common and may require early educational support.
Vision problems can occur from optic pathway gliomas; these tumors can cause reduced visual acuity or loss of visual field, usually in childhood. Seizures, headaches, and peripheral nerve pain also occur, especially if tumors compress neural structures.
Regular neurological and neuropsychological assessments help track progression and guide interventions like vision monitoring, therapy, and educational accommodations.
Tumor Development and Related Complications
You are at increased risk for benign nerve sheath tumors (neurofibromas) that arise along peripheral nerves; these include cutaneous, subcutaneous, and plexiform types. Plexiform neurofibromas can be congenital, grow deep along nerves, and cause pain, disfigurement, or functional impairment.
Some neurofibromas transform into malignant peripheral nerve sheath tumors (MPNST), though this is uncommon; watch for rapid growth, new persistent pain, or neurologic decline as warning signs. Other tumor-related complications include scoliosis from paraspinal lesions and localized bone dysplasia such as tibial bowing.
Imaging (MRI) and specialist evaluation guide treatment decisions, which range from monitoring to surgery or targeted medical therapy when tumors cause significant symptoms.